 
Since distal deficits appear first in most peripheral neuropathies, comparing proximal to distal sensation can help determine the location and extent of a lesion. Vibration sense is often the first sensation lost in peripheral neuropathy. Step 1: Strike the tuning fork with your palms so that it. 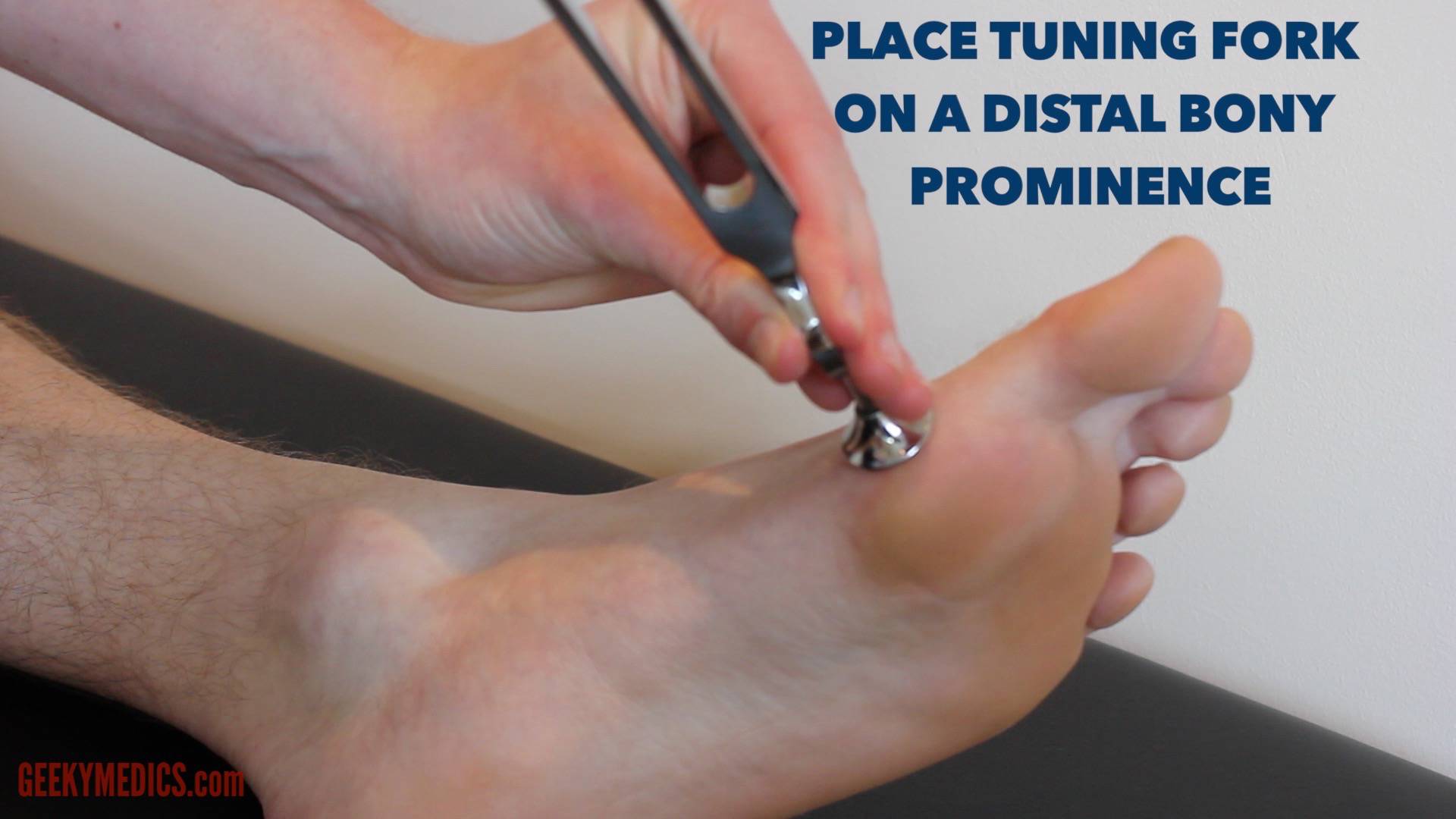
This pathway ascends ipsilaterally in the dorsal column to the gracile and cuneate nuclei in the medulla fibers then cross the midline and enter the medial lemniscus to ascend to the thalamus, and then to the somatosensory cortex. Vibratory sensation is often assessed using a 128-Hz tuning fork as seen in fig. Vibration and proprioception sensations are mediated by the dorsal column / medial lemniscus pathway. Therefore, the weighted prongs can be used for the diagnosing and monitoring associated with vibratory sensation, while the unweighted prongs are associated. If there is a deficit when testing a finger, testing of hand or forearm proprioception should be conducted to determine the extent of the deficit. Proprioception in fingers is tested by determining if the patient (with eyes closed) can sense whether a finger is being moved up or down. If there is decreased sensation distally, testing should also be done in other distal locations, as well as more proximally, to determine the extent of the deficit. Vibration sense is tested with a vibrating tuning fork placed over bony prominences of the feet (ankles) and hands (knuckles). Testing should be done initially distally. The vibration sense testing using a tuning fork was Performed. TENS units intensity ranges from 1 mA to 100 mA. Vibration sense testing with a 128-Hz tuning fork as a tool to determine recovery from epidural neuraxial block. Vibration is tested by sensation of a tuning fork held on a bony prominence. TENS probes were placed adjacent to the hallux. Upper extremity vibration and proprioception 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
